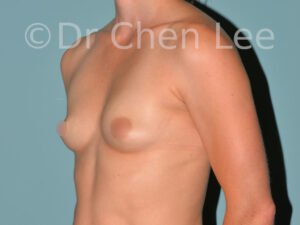
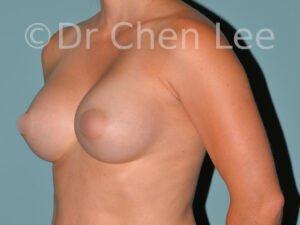
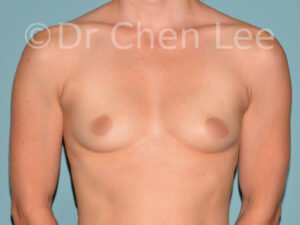
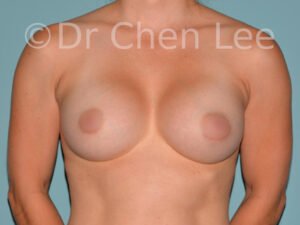
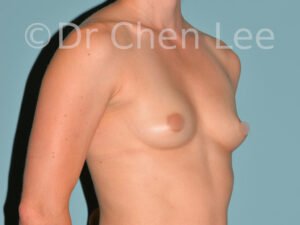
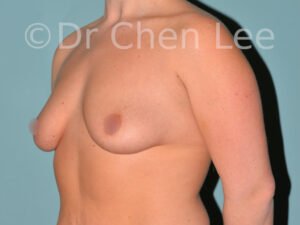
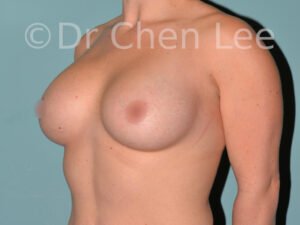
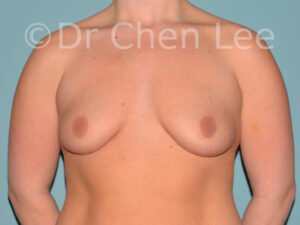
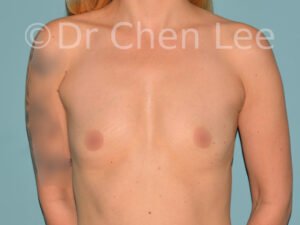
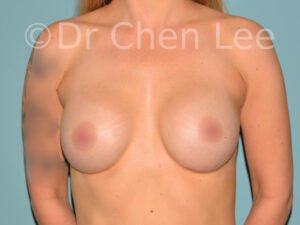
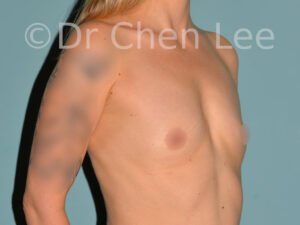
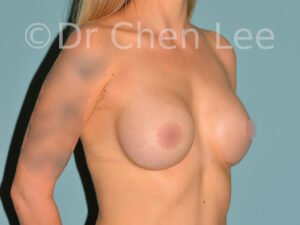
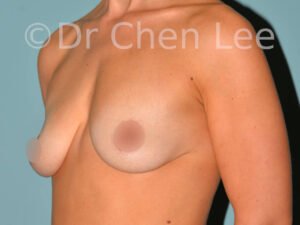
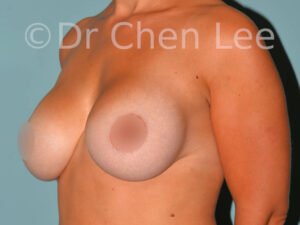
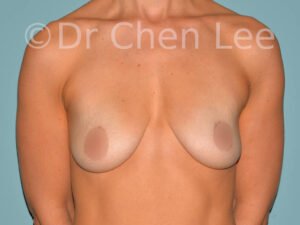
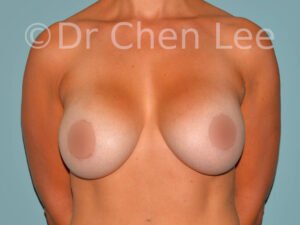
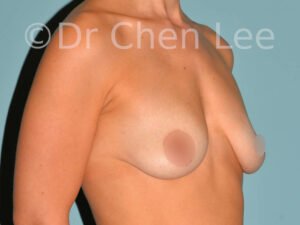
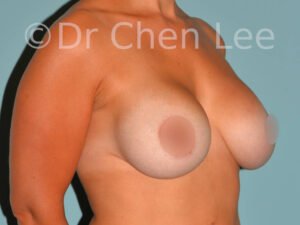
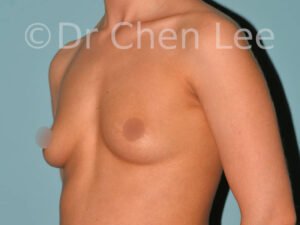
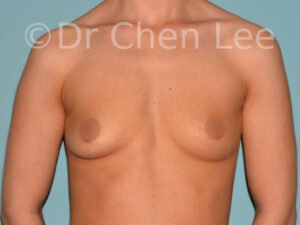
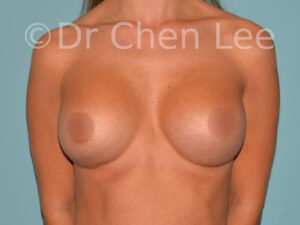
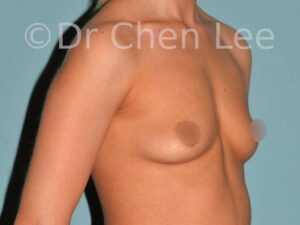
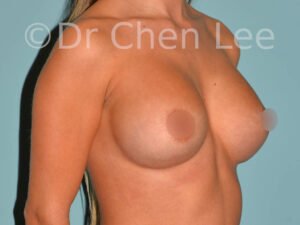
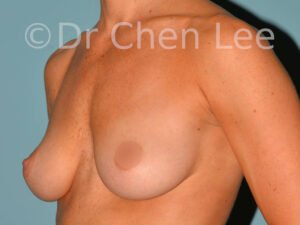
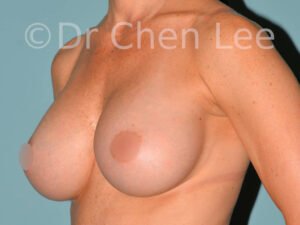
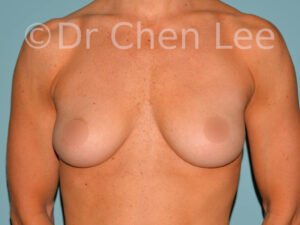
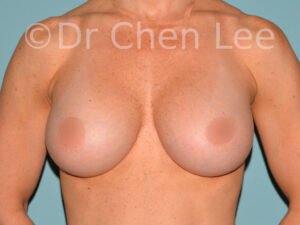
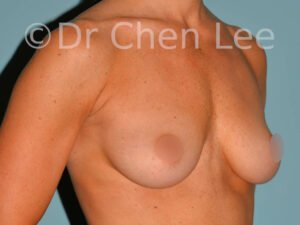
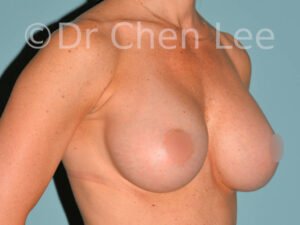
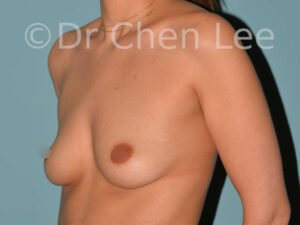
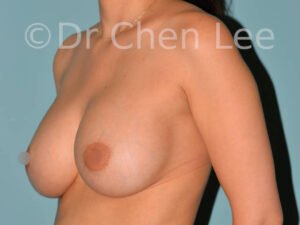
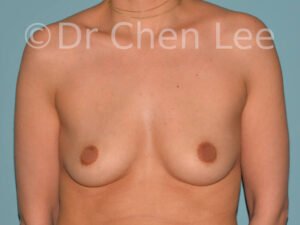
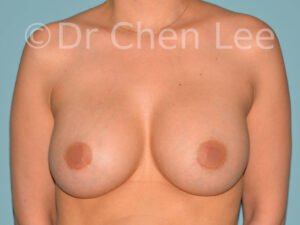
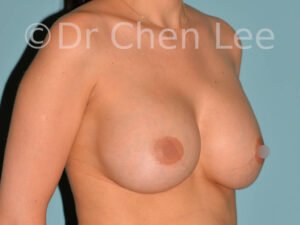
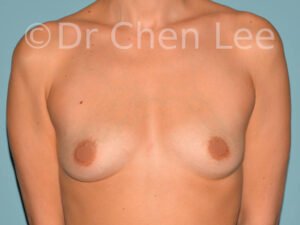
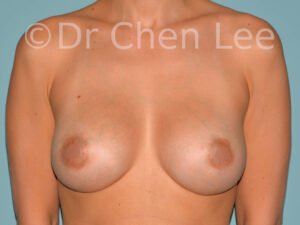
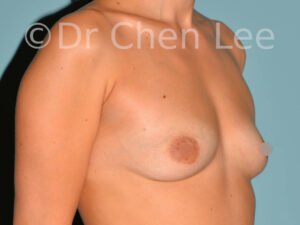
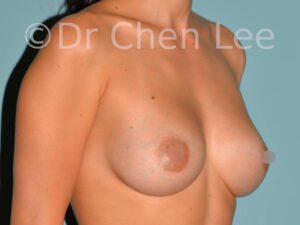
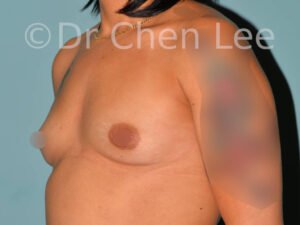
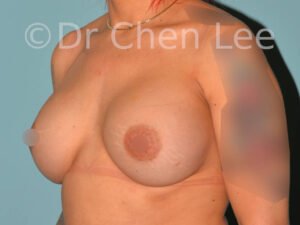
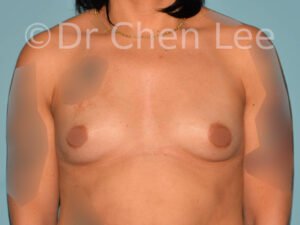
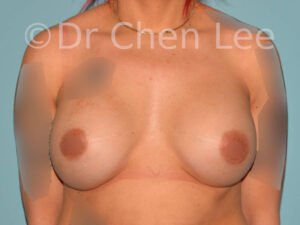
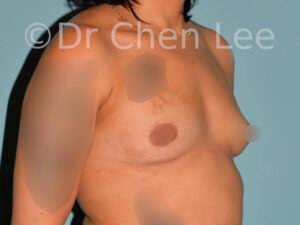
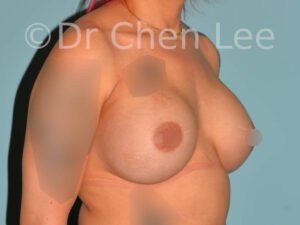
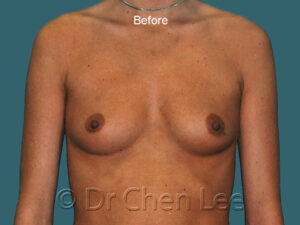
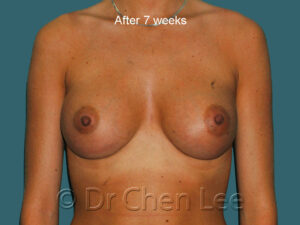
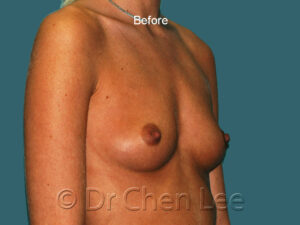
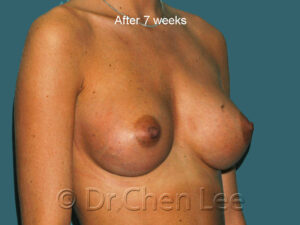
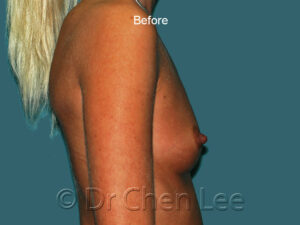
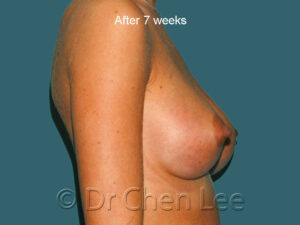
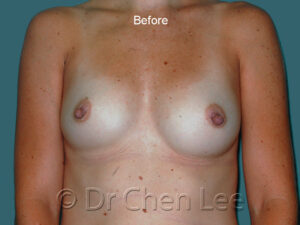
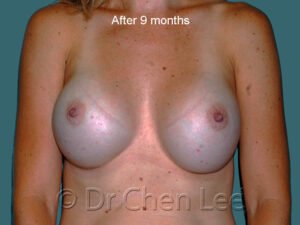
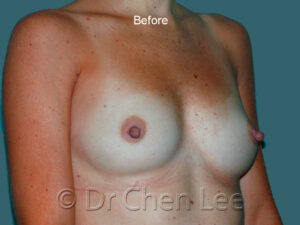
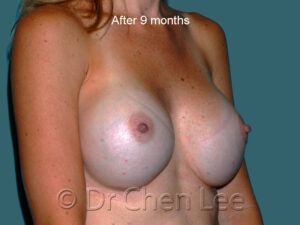
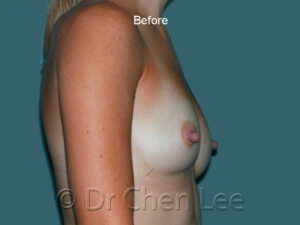
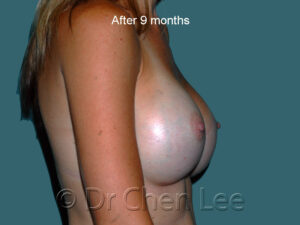
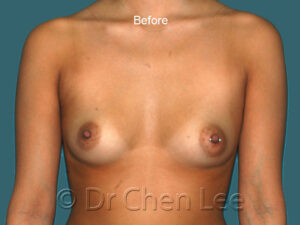
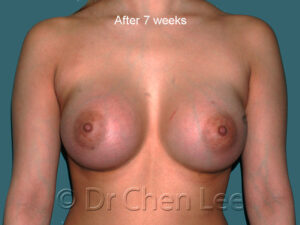
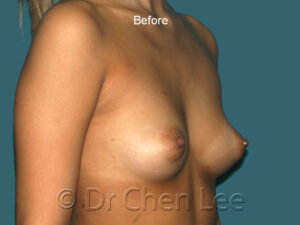
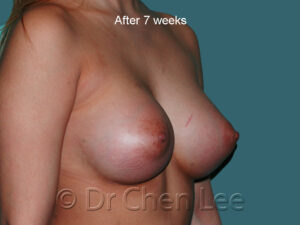
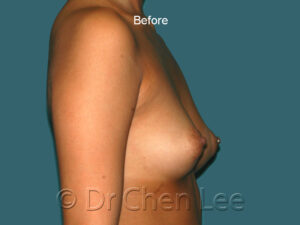
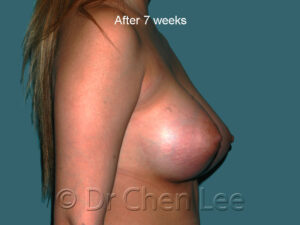
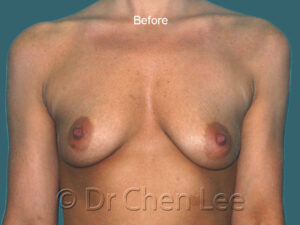
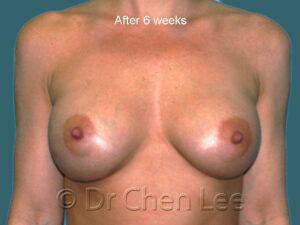
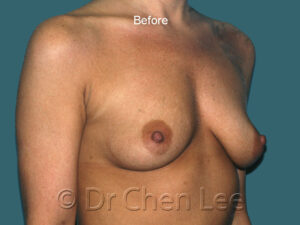
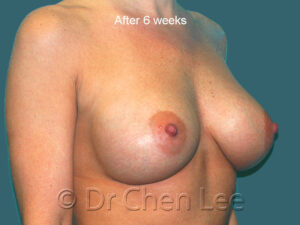
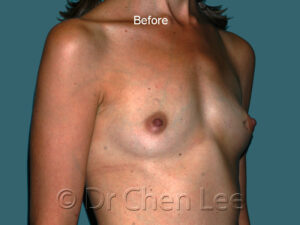
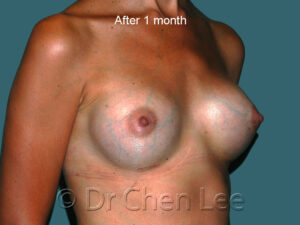
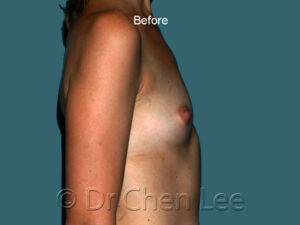
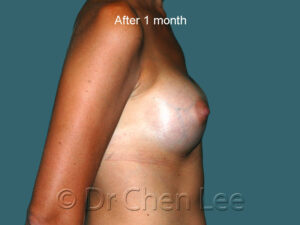
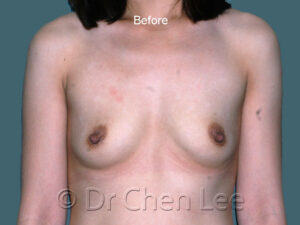
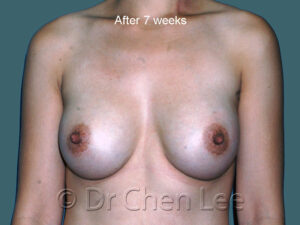
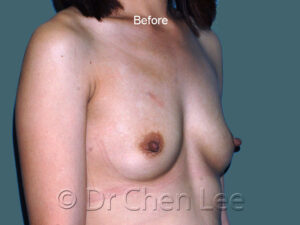
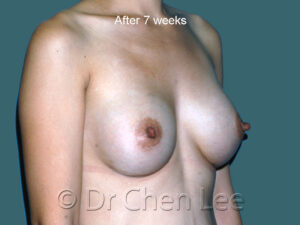
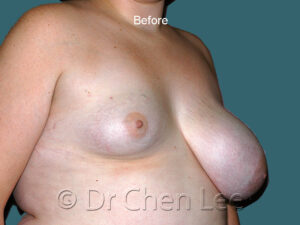
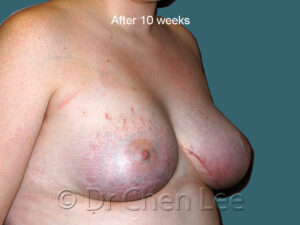
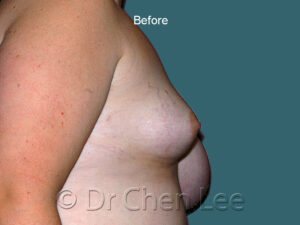
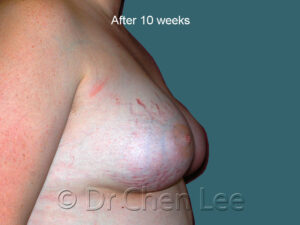
Breast Augmentation
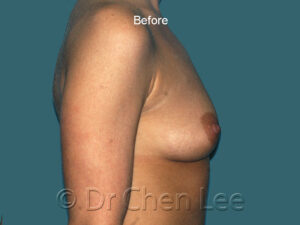
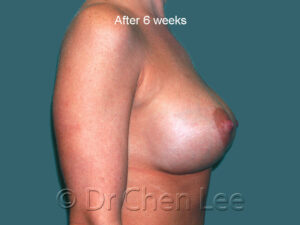
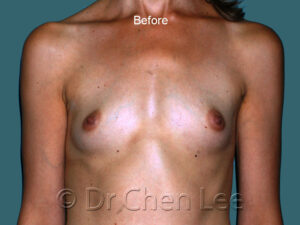
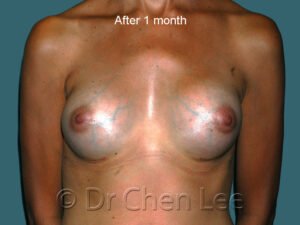
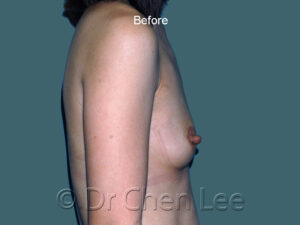
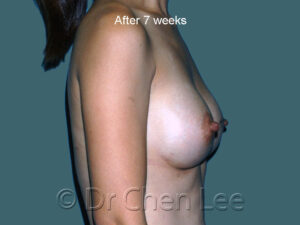
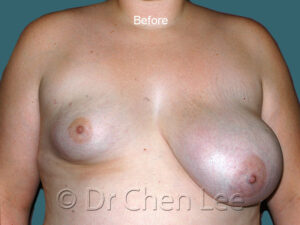
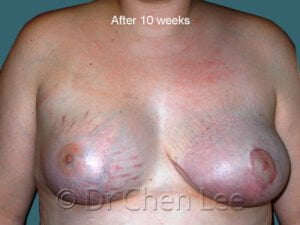
Breast augmentation in Montreal is the choice of those who wish to live life’s best experiences
For many women, breast size is an important part of feeling healthy, attractive, and confident. You can work hard to get fit and slim down, but if you aren’t born with the breasts you love, breast augmentation maybe your best option.
Breast Augmentation – The Essentials
Request a consultation to learn more about breast implants, breast augmentation techniques, recovery, and financing options. We look forward to helping you decide whether breast implants are right for you.
Breast Implants

Silicone breast implants are filled with a thick viscous gel composed of polymerized silicone. Its internal contents are designed to recreate the feel of a normal breast. Unlike the collapsible saline implant, a silicone breast implant comes from the manufacturer already pre-filled to a fixed volume. Direct surgical access through an infra-mammary or peri-areolar incision is required to position a silicone breast implant. The newest silicone “cohesive” gel breast implants better preserve the desired shape of the breast implant creating a fuller and more natural-looking breast. In Montreal, silicone cohesive gel breast implants are the most popular choice among women choosing to have breast augmentation.
Saline breast implants are silicone rubber external shells engineered to be filled with a saltwater solution. The saline breast implant is prepared by the manufacturer and provided to your surgeon as an empty shell. At surgery, the empty saline implant is surgically placed through a short hidden incision and then filled to your desired volume. The advantage of a saline breast implant is its collapsible small size offers the breast augmentation patient a shorter incision, a great choice of incision methods, and a precise fill volume. However, the water-like qualities of saline leave many women dissatisfied with the “bag of water” unnatural feel and visible external “rippling” sometimes seen after saline breast augmentation.
Textured surface breast implants were removed from the Canadian market in May 2019.
In 2017, Health Canada initiated a review of Canadian cases of rare cancer associated with textured surface breast implants. This entity is known as breast implant-associated anaplastic large cell lymphoma (BIA-ALCL). It is lymphoma and not breast cancer. BIA-ALCL develops in the scar tissue around a breast implant. The incidence is low. The majority of cases have been associated with textured surface breast implants. To date, scientific reports indicate favorable outcomes when affected patients are treated by breast implant explantation with surgical excision of the surrounding capsule. As of 2019, the national consensus on treatment is to surgically remove the implant and its surrounding scar without delay in any woman developing BIA-ALCL.
When considering fat grafting as an option for breast enhancement, it is essential to understand the principles of the procedure, as well as the benefits and risks involved.
Breast lipofilling involves removing fat from an unwanted area of the body and transferring it to the breasts. The fat is removed by liposuction, filtered, and injected as a graft into your breasts. The surviving grafted fat lives a normal life cycle similar to natural breast fat. When the procedure is successful, the benefits are soft natural breasts without any foreign material.
Unfortunately, breast enhancement by using fat grafts is inconsistent. Typically, 30-40% of the grafted fat does not survive the journey. This limits the magnitude of volume enhancement. Additional drawbacks to breast lipofilling include the risk of breast irregularities and cysts resulting from non-surviving grafts of fat.
Breast Augmentation Techniques

An implant pocket created over the muscle by surgical elevation of the mammary gland is called a subglandular, submammary, or retroglandular breast augmentation. Advantages include less pain, better projection, and a breast implant that does not move with pectoral contraction. This pocket is perfect for women with robust tissues who choose silicone implants. However, the implant is more likely to be visible and palpable through the layer of the breast and skin. Therefore subglandular placement is not recommended for women with thin breast tissue and those who choose to use saline implants.
Pocket creation under the muscle is also known as a submuscular, subpectoral, dual plane, or retropectoral breast augmentation. The pocket is created between the major and minor pectoralis muscles. Advantages include better implant coverage. Both rippling and palpability are reduced with the added muscle cover. This is a good choice in thin patients or when saline breast augmentation is planned. Substantial postoperative pain and breast implant displacement with pectoral contraction are drawbacks.
In August 2011, Dr. Chen Lee introduced the use of the “Keller Funnel” into his breast augmentation practice. The advantages of using this new system are the no-touch technique, reduction of stress on the outer shell of the breast implant, shorter length of skin incision, and less trauma to the tissue. Ask Dr. Chen Lee how the Keller Funnel will benefit you.
Inframammary Incision:
The inframammary incision is the most common incision used for breast augmentation. This incision is located in the crease where the breast meets the chest and leaves a well-concealed scar below the breast. Direct visual access to the implantation site facilitates accurate breast implant placement with a low likelihood of malpositioning and asymmetry. All sizes of breast implants can be surgically positioned through an inframammary incision. This incision is particularly suitable for larger-sized silicone breast implants.
Periareolar Incision:
The periareolar incision is located on the lower border of the pigmented skin surrounding the nipple (lower margin of the areola). A natural pigmentation change between the areola and normal skin serves to camouflage and conceal the resulting breast augmentation scar. This access incision also permits direct visualization of the surgical pocket for final silicone breast implant placement. The length of the periareolar incision is limited by the circumference and size of the areola. Not all sizes of silicone breast implants can be placed through this incision.
Transaxillary Incision:
The transaxillary incision is hidden in the armpit and is remotely located from the breast. A collapsible saline breast implant is preferred with this incision. The smaller dimension of the deflated saline breast implant facilitates its positioning through the tight confines of this remote incision. The implant is filled at surgery only after manipulation into its desired position. Modest or smaller-sized prefilled silicone smooth breast implants can also be positioned through the transaxillary incision. Direct surgical access for pocket creation is not possible. The creation of a well-contoured symmetric lower breast pole remains a problem with remote transaxillary access. The resulting scar in the armpit might be visible with sleeveless attire. Women who often wear sleeveless apparel might consider another choice of incision for their breast augmentation.
Breast Implant Cost

$165.25 + taxes
The initial office consultation for breast augmentation is a wonderful opportunity to establish a healthy patient-surgeon relationship. During the consultation, the plastic surgeon will typically perform a breast exam, recommend a technique specific to your case, and discuss the types of skin incisions, and placement of the breast implants. In addition, the risks associated with breast augmentation will be explained and given in writing. For the patient, she should use this initial encounter to judge the professionalism and qualification of the doctor, as well as the quality of the information transmitted. With a comprehensive understanding of your goals, the plastic surgeon will be better able to achieve your objectives and make your breast augmentation journey safe and satisfying.
$10,800 + taxes
The price of breast augmentation in Montreal is quoted as a “global fee”. The price quote includes costs of the surgeon, anesthesiologist, nurses, breast implants, office visits during the first postoperative year, operating room, and surgical facility fees. Revisions and touch-up surgeries are not included in the initial breast augmentation quotation. If general anesthesia is necessary, you will have to pay for the substantial costs associated with a surgical revision. Minor touch-up surgery under local anesthesia can often be performed at minimal expense. The customary price of breast augmentation in Montreal is $10,800 + taxes.
Surgeries are payable in cash, certified checks (bank drafts) or Interac. We also work with an independent credit company that offers financial payment plans for cosmetic surgery procedures. However, you should be aware that the interest rates and administration fees of this specialized company are higher than traditional financial institutions. It is often better to negotiate a loan through your personal bank or financial institution. We encourage you to do your homework and compare the true financial cost of these various financial options.
Scheduling your breast augmentation is a 3-step process.
Step 1: Reservation Date for Surgery
Our office staff works diligently to schedule surgeries to your availability and preference. However, operating room resources are precious and a financial commitment is necessary to reserve a dedicated time. Half of the surgical fee is due upon reservation of dedicated operating room time for your breast augmentation. Full payment is due 2 weeks before the day of surgery.
Step 2: Breast Implant Sizing
Once your surgery is scheduled, our office will work with you to choose the ideal breast implant size for your body. This often requires several in-office visits where you are able to place implant sizers under clothing to simulate the results expected. It often helps to have a family member or friend present during your breast implant sizing visits. Breast implant sizes must be chosen well before surgery so that we have sufficient time to order and have your preferred breast implant sizes available at the surgery.
Step 3: General Health Evaluation
Breast augmentation is performed under general anesthesia. To ensure your safety, a general physical examination and laboratory tests are performed. During your preoperative visit, our breast surgeon will obtain standardized medical photos and provide general instructions on preparation for surgery and pain management.
FAQ – BREAST AUGMENTATION
Most breast implant surgeries are completed in 1 hour and women are able to return to their normal activities (with certain restrictions) after a few days. At Cosmetic Surgery Montreal, breast augmentation procedures are performed on ambulatory outpatients under general anesthesia.
It is natural to have concerns and questions regarding breast implant safety. Dr. Chen Lee is committed to helping you understand the risks to make an informed decision about breast augmentation.
Many women desire an increase in the size of their breasts. If you are one of those women and are 18-years-old or older, physically healthy, emotionally stable, and have realistic expectations of what plastic surgery can accomplish, you are probably a good candidate for breast augmentation.
The best way to determine with certainty if a breast augmentation is appropriate for you is to meet with a reputable board-certified plastic surgeon.
Your plastic surgeon will guide you through the preparation. You will need to decide on several important breast implant (type, size, incision, placement) decisions. Once these decisions are finalized, a surgery date is reserved at the surgery center. Preoperative laboratory tests are also ordered to ensure that you are fit to have surgery under general anesthesia. You will also be provided pre-surgical instructions on medications, smoking cessation, alcohol use, etc.
The best method to choose your implants starts by having a thorough discussion with your plastic surgeon. Your body type and desired objectives are important considerations in choosing breast implants to use for your breast augmentation. In our plastic surgery practice, the plastic surgeon uses your unique body shape and “in-office” sizing to assist in the selection of breast implants to better achieve your breast augmentation goals.
While the anticipated change expected with breast augmentation is exciting, it is important to be aware of the risks and potential complications. Surgery and general anesthesia are always accompanied by some risks to your general health. Although rare, there even exists the possibility of death.
A partial list of potential complications associated specifically with breast augmentation includes asymmetry, deformation, infection, bleeding, delayed healing, reoperation, implant visibility, implant palpability, pain, loss of sensation, scars, capsular contracture, implant rupture, implant malposition, and no guarantee to the final size.
Following breast augmentation, patients often experience temporary loss of erotic and general sensitivity to the breasts and nipples. In most instances, normal sensation returns spontaneously and naturally over time.
Modern techniques of breast augmentation do not harm the breast tissue and will not alter your ability to lactate and produce breast milk. Your ability to breastfeed following surgical placement of breast implants should not be affected.
Recovery is different for everyone. In general, most women can get up and walk alone the day after surgery. However, it is important to avoid most of your usual activities such as cooking, cleaning, carrying weight (groceries or children), and driving for 7 to 14 days. You will be advised to wait several weeks before resuming exercise.
We strongly recommend a minimum of 2 weeks away from work. On occasion, some patients may be able to return to light nonphysical work (e.g. office) 7 to 10 days after breast augmentation. Every patient’s experience is unique. The size and position of implant placement may affect the above recommendations.
Modern breast implants are expected to last for many years. However, the actual long-term durability has not been scientifically defined. While many patients believe that their breasts are permanently augmented with a single surgery, implantable synthetic prostheses should not be considered lifetime medical devices. All synthetic implantable medical devices (such as heart valves, brain shunts, orthopedic joints, and breast implants) can malfunction and fail.
While the risk of breast cancer is not elevated following breast augmentation, screening is still necessary and encouraged. Common methods for detecting breast cancer include mammography, ultrasound, and magnetic resonance imaging (MRI). Mammograms can still be performed, however, modified techniques such as breast compression to enhance the view of the breast tissue is often necessary for an effective breast mammogram. To better plan, your breast investigations, the physician managing your breast cancer prevention routine should be made aware of your breast augmentation.
In 2017, Health Canada initiated a review of Canadian cases of rare cancer associated with textured surface breast implants. This entity is known as breast implant-associated anaplastic large cell lymphoma (BIA-ALCL). It is lymphoma and not breast cancer. BIA-ALCL develops in the scar tissue around a breast implant. The incidence is low. The majority of cases have been associated with textured surface breast implants. To date, scientific reports indicate favorable outcomes when affected patients are treated by breast implant explantation with surgical excision of the surrounding capsule. As of 2019, the national consensus on treatment is to surgically remove the implant and its surrounding scar without delay in any woman developing BIA-ALCL.
Textured surface breast implants were removed from the Canadian market in May 2019.
Breast Augmentation Price
- $10,800 + taxes
- Includes professional fees (surgeon, anesthesiologist, and nurses)
- Includes the surgical facility and operating room expenses
- Includes silicone or saline-filled breast implants
- Revisions and touch-up surgeries are not included
Preparation for Breast Implants
- Avoid nonsteroidal anti-inflammatory medications (Aspirin, Advil, etc.)
- Stop smoking, do not use e-cigarettes, avoid nicotine and marijuana
- Do not drink alcohol
- Continue prescription medications (unless advised otherwise)
Day of Surgery
- Stay fasted from midnight prior to surgery (no food, no drinks)
- Be punctual – Arrive on time at the surgery facility
- Wear loose clothing – Avoid the use of cosmetics
- Come accompanied by a responsible person (transportation home)
Advice After Breast Implants
- Do not cook, clean, carry weight (groceries or children), or drive
- Take your medications as prescribed
- Notify us promptly of unexpected symptomatology
- Do your best to rest and relax for 2 weeks